The nomenclature of these nuclei is complex and there are short pithy acronyms for a very large number of structures, as needed to succinctly label diagrams and sections. top below), is the corticospinal tract (pyramidal tract below). Quite far away from the vestibular nuclei, in the front (i.e. Also in the medulla (besides the vestibular nucleus) is the spinal tract of V (accounting for facial numbness), the nucleus ambiguus (accounting for swallowing problems), the spinothalamic tract (contralateral numbness), and the lower portion of the inferior cerebellar peduncle as well as spinocerebellar connecting tracts (ipsilateral clumsiness). 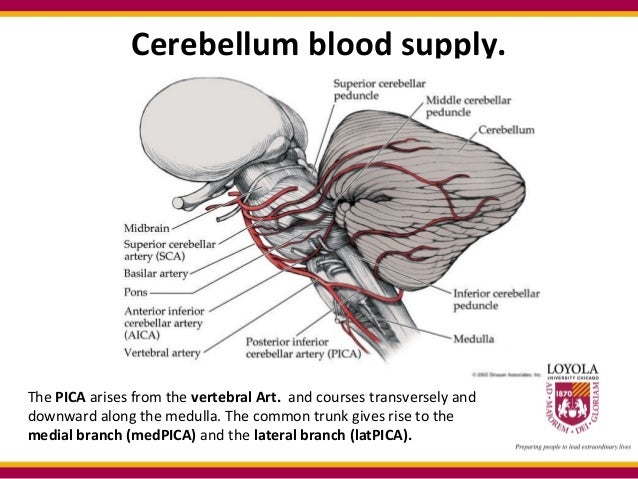
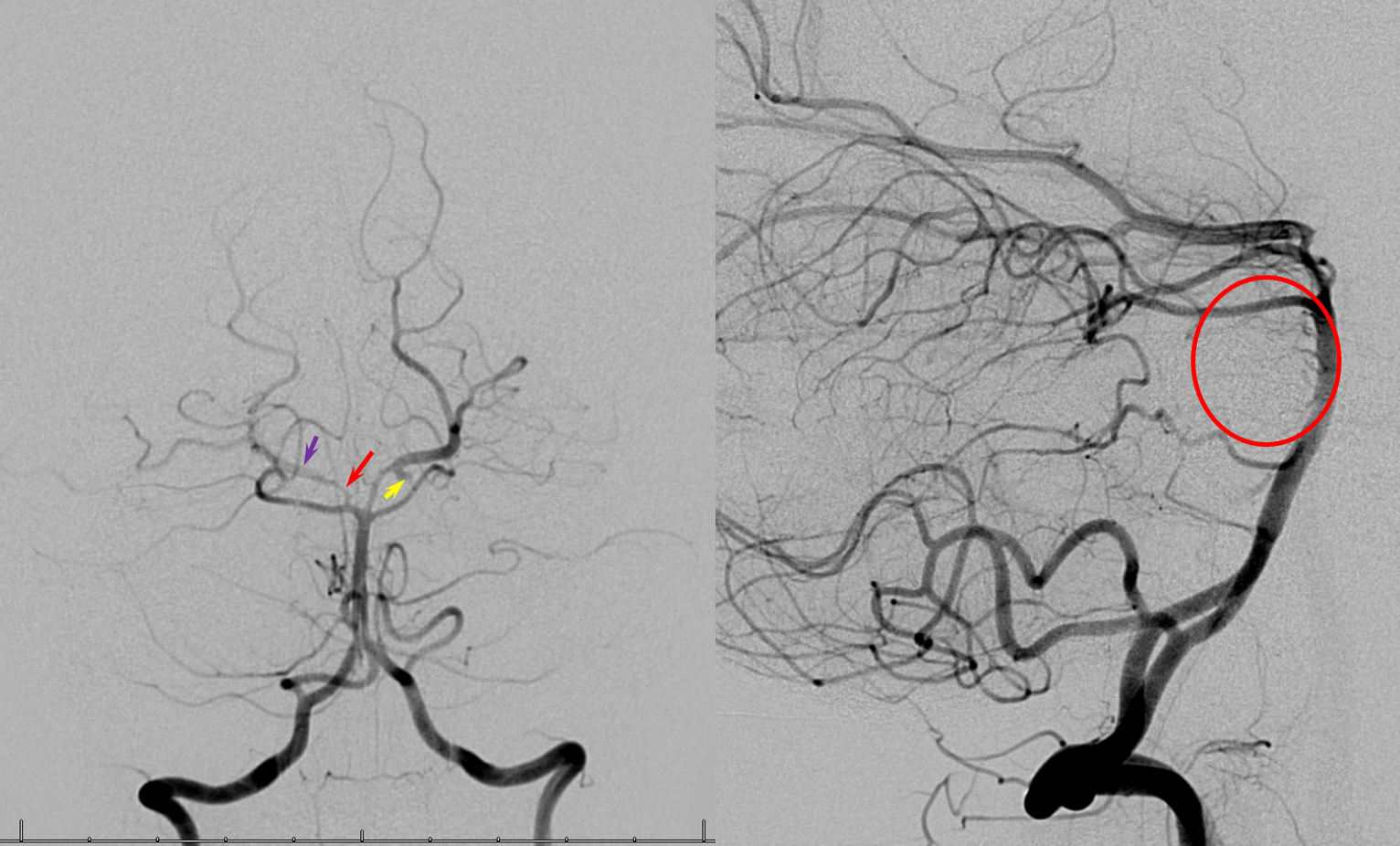
Thus there is a lot of room for variation in the areas of damage. As the diagram illustrates above, the vestibular nucleus which extends from lower pons into medulla, is also a big target because of it's length. It is about 3 cm in length and 2cm in greatest diameter, and is a big target. The medulla is the portion of the brainstem just below the pons (recognized by cerebellar peduncles), and the first cervical spinal nerve (C1). PICA is also the most common site of occlusion from propagating thrombus or embolism caused by injury to the third section of the vertebral artery, and Wallenberg's syndrome is the most common stroke caused by chiropractic manipulation (Caplan, 1986). Of these strokes, while dissection causes 15% (Kim, 2003). Because of the far more common origin from the vertebral artery, most "PICA" syndrome strokes actually areĭue to vertebral artery occlusion (Kim 2003). PICA may arise from the vertebral artery (the usual case), or as a separate branch of the basilarĪrtery. Usually LMS/Wallenberg's is caused by loss of blood flow in the posterior inferior cerebellar artery (PICA). Source of figure: what-when-how neuroscience. The "VN" is the inferior vestibular nucleus, more commonly labeled as either DVN or IVN. SVN,LVN,MVN are the superior,lateral and medial vestibular nuclei. It both supplies the medulla as well as the inferior cerebellum.Ĭentral vestibular pathways, drawn from back of brainstem with cerebellum removed. PICA is usually a branch of the vertebral artery. What causes Wallenberg's/Lateral Medullary syndrome ? Hearing symptoms are generally from strokes in the territory of he next higher artery in the brainstem, the anterior inferior cerebellar artery or AICA. LMS generally does not include hearing symptoms however. Opposite side weakness (Babinski-Nageotte) Sympathetic connections descending from hypothalmus into cervical cord. These were divided up into the upper group (rostral) and the more common lower group (caudal). Kim (2003) provided a table including 18 symptoms (or categories) of symptoms. 
In addition, there are a lot of important structures supplied by PICA, and depending where the damage lies, there may be other findings. With LMS almost always have a Horner's syndrome (acutely unilateral ptosis, miosis and facial anhidrosis), but partial Wallenberg's are more the rule than the exception. 
Very well and often resume their previous activities (Nelles et al, 1998). Hemiataxia, dysarthria, ptosis and miosis. Or "Wallenberg's syndrome", after Wallenberg's description in 1895. The PICAstroke syndrome is also known as "lateral medullary syndrome", All rights reserved.PICA (posterior cerebellar artery syndrome). We suggest that performing MRI and MRA in the early stage of AICA syndrome is important for distinguishing cerebellar infarction resulting from vestibular disease.Ĭopyright © 2011 Elsevier Ireland Ltd. Consequently, the patient was diagnosed with AICA syndrome but demonstrated regression following steroid and edaravone treatment. MRI and MRA revealed infarction of the right cerebellar hemisphere indicating occlusion of the AICA. The patient's brain was examined by magnetic resonance imaging (MRI) and magnetic resonance angioglaphy (MRA) and showed an infarction localized in the pons and cerebellum. An eye tracking test (ETT) and optokinetic pattern test (OKP) showed centralis abnormality. However, right peripheral facial palsy appeared 2 days later. Initially, we diagnosed the patient for sudden deafness with vertigo. Otoneurological examinations showed sensorineural hearing loss of the right ear and horizontal and rotatory gaze nystagmus toward the left side, and a caloric reflex test demonstrated canal paresis. Spontaneous nystagmus toward the left side was also observed. An audiogram revealed a severe hearing loss at all tested frequencies in the right ear. A 39-year-old female presented with vertigo and sudden hearing loss, tinnitus, and aural fullness of the right ear. We report a case of infarction of the anterior inferior cerebellar artery (AICA) with peripheral facial palsy following vertigo and acute sensorineural hearing loss.
0 Comments
Leave a Reply. |

 RSS Feed
RSS Feed
